Prostate Cancer

At Riverstone Urology in Cypress, Dr. Russell Libby focuses on early detection, clear explanations, and treatment plans that match your cancer risk and your goals for quality of life. He has extensive experience with robotic prostate surgery and works closely with radiation and medical oncology partners when a combined approach makes sense.
What Is Prostate Cancer?
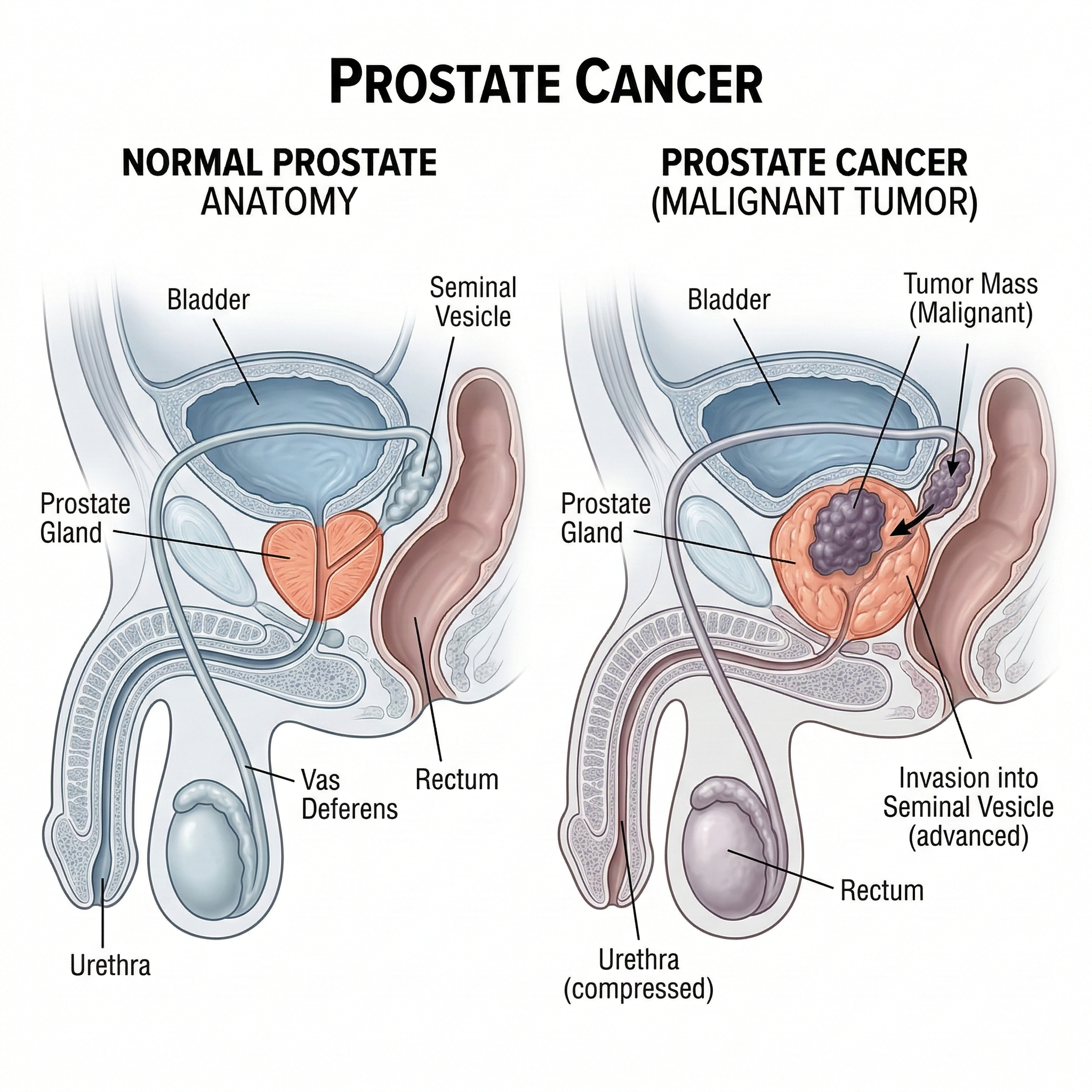
Most prostate cancers are adenocarcinomas that grow from the gland cells inside the prostate. Many grow slowly and stay in the gland for years. Others behave more aggressively and spread outside the prostate to lymph nodes and bone. Early detection gives more options and often better long term control.

Risk Factors
Your Risk For Prostate Cancer Goes Up With:
- Age: Risk rises sharply after age 50. Most cases appear after age 65.
- Family history: A father, brother, or multiple relatives with prostate cancer increases risk. Certain inherited gene changes, such as BRCA2, raise risk further.
- Race: Black men face higher risk of diagnosis and higher risk of aggressive disease.
- PSA pattern over time: Higher PSA at a younger age links to higher lifetime risk of prostate cancer and prostate cancer death.
- Other factors: Obesity, low activity level, and some dietary patterns link to higher risk in research, although those links are not as strong as age and family history.
Symptoms
When Symptoms Appear, They Can Include:
- Weak or slow urine stream
- Trouble starting or stopping urine
- Frequent urination, especially at night
- Feeling that your bladder does not empty completely
- Pain or burning with urination
- Blood in urine or semen
- New erectile dysfunction
- Pain in the hips, back, or ribs, especially with advanced disease

Screening And Early Detection
Screening aims to find prostate cancer before symptoms appear. Common tools include:
- PSA blood test
- Digital rectal exam, DRE
For this reason, major groups recommend shared decision making instead of automatic screening for everyone. You talk with your doctor about your risk, values, and concerns, then decide together when to start PSA testing and how often to repeat it.
At Riverstone Urology, Dr. Libby:
- Reviews your age, family history, race, and other risk factors
- Looks at your PSA level and how it changes over time
- Explains the pros and cons of biopsy or continued monitoring
- Uses MRI and targeted biopsy techniques when appropriate, to focus testing on areas of real concern
How Prostate Cancer Is Diagnosed
If Your Psa Or Exam Looks Concerning, Dr. Libby May Suggest Further Testing. Typical Steps Include:
Repeat PSA And Exam
Prostate MRI
Prostate Biopsy
Under ultrasound and often MRI guidance, Dr. Libby takes small samples from specific regions of the prostate. A pathologist reviews these samples under the microscope.
The report describes:
- Presence or absence of cancer
- Gleason score and Grade Group, which tell how aggressive the cells look
- Number and percentage of cores involved
Risk Groups And Staging
Prostate Cancer Care Uses Risk Groups To Guide Treatment. These Groups Combine:
- PSA level
- Gleason score and Grade Group
- Number of biopsy cores with cancer
- MRI findings
- Evidence of spread on imaging
Broad Groups Include:
- Low risk
- Favorable intermediate risk
- Unfavorable intermediate risk
- High risk
- Very high risk or metastatic disease
Treatment Options At Riverstone Urology
Active Surveillance
For many men with low risk prostate cancer, immediate treatment is not required. Instead, Dr. Libby may recommend:
Regular PSA testing
Periodic MRI
Repeat biopsies at defined intervals
Robotic Radical Prostatectomy
Surgery removes the entire prostate and seminal vesicles, then reconnects the bladder to the urethra. At Riverstone Urology, Dr. Libby performs this operation with robotic assistance in appropriate patients.
Benefits of a robotic approach often include:
- Smaller incisions
- Less blood loss
- Shorter hospital stay
- Faster return to regular activity
Radiation Therapy
Radiation uses high energy beams or seeds to destroy cancer cells. Dr. Libby partners with radiation oncology colleagues for:
- External beam radiation
- Brachytherapy with implanted radioactive seeds
Hormone Therapy
Prostate cancer cells depend on testosterone for growth. Hormone therapy lowers or blocks testosterone to slow or shrink cancer. Options include:
- Injections that signal the body to stop making testosterone
- Medicines that block testosterone action
- In some cases, surgery to remove testosterone producing cells in the testicles
Other Systemic Treatments
For advanced or recurrent prostate cancer, Dr. Libby works with medical oncology to introduce:
- Chemotherapy
- Newer hormone drugs
- Targeted therapies and immunotherapies in selected cases

Side Effects And Quality Of Life
Prostate Cancer Treatment Affects Urinary Control, Erections, And Sometimes Bowel Function. Common Side Effects Across Treatments Include:
- Leakage of urine, especially in the early period after surgery
- Changes in erections and orgasm
- Dry orgasm after surgery, with no semen
- Bowel urgency or discomfort after radiation
- Hot flashes, fatigue, and metabolic changes with hormone therapy
Side Effects And Quality Of Life
Prostate Cancer Treatment Affects Urinary Control, Erections, And Sometimes Bowel Function. Common Side Effects Across Treatments Include:
- Leakage of urine, especially in the early period after surgery
- Changes in erections and orgasm
- Dry orgasm after surgery, with no semen
- Bowel urgency or discomfort after radiation
- Hot flashes, fatigue, and metabolic changes with hormone therapy
Prostate Cancer Care With Dr. Libby In Cypress
When You See Dr. Libby For Prostate Cancer, You Can Expect:
- Clear explanations in plain language
- A review of all reasonable options for your stage and risk group
- A strong focus on early detection when risk is high
- Advanced surgical options, including robotic prostatectomy
- Coordination with radiation and medical oncology when combined therapy offers the best control
